Definition
Spina bifida (SB) is a congenital defect that occurs when the bones of vertebral columns do not form or fuse completely around some part of kid’s spinal cord. In mild cases it only affects the appearance of the skin of the lower back while in severe cases spina bifida children are not able to walk and perform daily activities without support [1,4].
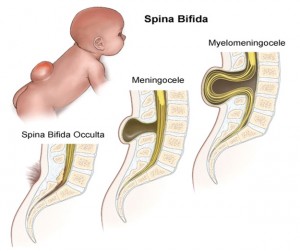
Different forms of Spina bifida
Depending upon the various anatomical defects in vertebral column closure, SB can be divided into various forms [2]. These types include:
- Mild case/form (Spina Bifida Occulta) – a mild form is seen more often as compared to other forms. Usually this type of SB does not lead to any problem and requires no treatment. You cannot even see this defect, and it is accidentally found if the patient has a X-ray of lower back for another reason [4].
- The severe forms are less common as compared to mild ones. Depending upon the size and type of the defect, the severe variety of SB can be classified into two types. These include:
-
- Meningocele– In this defect only meninges of the spinal cord are protruded out through the bony defect without containing spinal cord contents. Clinically, children with SB of this variety present with a cystic swelling on the lower back usually without any other complaint [7].
- Myelomeningocele– This is the rarest form of SB. This is the actual form of SB that the layman calls “Spina Bifida”. It is the most severe type of SB. Here, the defect in vertebral column involves the spinal cord meninges along with some contents of the spinal cord. So in this form, the chances of damage to spinal nerves and other parts of the spinal cord are more likely as compared to those with meningocele. kids with SB having this form of defect, usually present clinically with cystic bulging in their lower back, urinary and bowel complaints and poor coordination. In some cases the skin over the lower back swelling is open and spinal nerves are exposed [5].
Causes and Risk Factors
The exact cause of SB is still under debate. Researchers believe that genetic and environmental factors are part of cause. Women who previously gave birth to a spina bifida kid, are more likely to have another kid with this anomaly. Decreased intake of folic acid, obesity and diabetes are the probable risks factors for development of SB [3,4].
Clinical presentation
The signs and symptoms of the disease depend upon the severity of the defect. When the defect is mild there may be no signs or symptoms and such defect can only be picked up by a radiograph of the lower back. These kids may have asymptomatic hairy patch or dimple on their back in mild cases. In severe cases, the spinal nerves are usually damaged so the child may present with many complex signs and symptoms. These include:
- Paralysis of lower limbs
- Numbness of lower limbs
- Pain and heaviness in lower limbs
- Loss of sensation in peri-anal and genital area
- Difficulty in walking
- Poor coordination in walking
- Urinary frequency, urgency and incontinence
- Urinary retention
- Constipation and diarrhea
- Scoliosis
- Some kids may also develop hydrocephalus. It can cause seizures, intellectual disability and sight problems.
- An allergy to latex (a type rubber) is reported in many children with severe forms of SB [6].
Spina Bifids Kids Diagnosis
SB before delivery of the infant can be diagnosed in pregnant women with help of the following tests:
- Maternal serum triple or quadruple screen
- Ultrasonography
If results of the above tests suggest any birth anomaly, amniocentesis can be performed to confirm the presence of SB in the baby. After birth, the diagnosis can be made with the help of followings:
- Presence of hairy patch or dimple on lower back of the child
- Presence of cystic swelling on lower back of the kid
- Presence of cystic swelling along with signs and symptoms of SB
- X-ray lower back
- CT-Scan or MRI of spinal cord [2]
Treatment
The treatment plan depends upon the severity of the problem. In mild cases, no treatment is needed while the kids with severe form of defect may need surgery. The child may also require physiotherapy and other aids as well. The following points are important regarding the support of a spina bifida kid [8]:
- Provide the child with fresh and healthy food
- Do regular doctor visits
- Keep the child away from latex products
- Use proper catheterization in care of infection in case of urinary complaints
- Have physiotherapy of lower limbs
- Take care of bowels
- Use proper nursing care and posture change in cases of paralysis to prevent bed sores [5,7]
A first-time mom explains the challenges of raising a child with SB
Prevention
It can be prevented by the following steps:
- Pregnant mothers should have a high intake of food which is rich in folic acid
- Avoidance of teratogenic drugs during pregnancy
- Early miscarriage if needed after proper concealing [5,7]
Conclusion
SB is a congenital defect that can be divided into mild and severe forms. Mild cases are usually asymptomatic and need no treatment. Severe cases may present with complex signs and symptoms and may require surgical intervention. SB can be prevented by intake of folic acid in the diet and avoidance of drugs during pregnancy. The possibility of an abortion can be offered to the mother after explaining the outcome of SB.
[ois skin=”1″]References
- Mitchell LE, Adzick NS, Melchionne J, et al. Spina bifida. Lancet 2004, 20-26;364(9448):1885-95.
- Fletcher JM, Brei TM. Introduction: Spina Bifida—A Multidisciplinary Perspective. Dev Disabil Res Rev 2010:16(1):1-5.
- Groenen PM, Klootwijk R, Schijvenaars MM, et al. Spina bifida and genetic factors related to myo-inositol, glucose, and zinc. Mol Genet Metab 2004 Jun;82(2):154-61.
- Forres DM. Spina Bifida. Proc R Soc Med 1977 ; 70(10): 743–4.
- Myelomeningocele [Internet]. [Last updated 15 March 2004; Cited on 30 Oct 2013]. Available from: http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0002525/.
- Sandler AD. Children with spina bifida: key clinical issues. Pediatr Clin North Am. 2010;57(4):879-92.
- Rossi R, Alexander M, Cuccurullo S. Physical Medicine and Rehabilitation Board Review. [Internet]. [Last updated 2004; Cited on 30 Oct 2013]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK27180/.
- Ahrens K, Yazdy MM, Mitchell AA, Wereler MM. Folic acid intake and spina bifida in the era of dietary folic acid fortification. Epidemiology 2011 Sep;22(5):731-7.
Related Articles:



