Overview
Hydrocephalus refers to accumulation of excessive cerebrospinal fluid (CSF) around the brain due to a pathway obstruction or poor absorption. CSF is synthesized by choroid plexus in the ventricular system of the brain and it functions to protect the brain and spinal cord matter. In simple words, CSF around the brain offers a cushion effect and prevents brain from injuries. Excessive amounts of CSF either due to its pathway obstruction or its poor absorption can lead to increased intracranial pressure, thus resulting in life threatening consequences.
In most cases it is easy for doctors to diagnose it, while in some cases it is impossible to diagnose because of a very small amount of CSF accumulation or the presence of minimal signs and symptoms [1,2]. The most common treatment for this condition is placement of a tube, called a hydrocephalus shunt to bypass extra CSF from the head to another place in the body where it can be removed naturally. It consist of valves to regulate direction as well as quantity of fluid to be removed/drained. They contain 3 parts, that is:
- A catheter that reaches the area of brain where there is excessive CSF
- A valve to regulate the CSF flow
- A tubing system that carries fluid from one place in the body to another [3].
Various Types of Hydrocephalus shunts
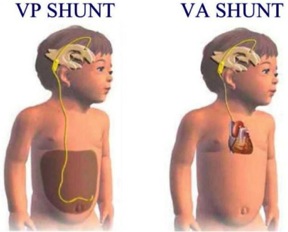
There are many types but the most common type is the ventriculo-peritoneal (VP) shunt. This functions to remove Cerebrospinal fluid (CSF) from the ventricle and sends it to the body’s abdomen. Other less common types are:
- Ventriculo-atrial (VA) shunts- This removes the CSF from ventricle and sends it to a vein, usually present in the neck or under the collarbone
- Ventriculo-pleural shunts- It removes CSF from ventricle and sends it to the pleura around the lungs
- Ventriculo-gall bladder shunts- it serves to drain CSF from ventricle to the gall bladder [3].
Video of what it looks like
Shunt valves
All of them work by regulating the quantity of CSF that is to be drained. Most of these work automatically when intracranial fluid pressure in the head gets very high. Some valves may have special devices to avoid excessive drainage of CSF from the ventricles [4].
Place of hydrocephalus shunt insertion
Experts are still unable to decide which type is the best for whom. Therefore, neurosurgeons usually select ones that they think are the best. The locations in the head where they can be placed are:
- The back of the head
- The edge of the soft spot
- Above and behind the ear
It is also difficult for experts to decide on which one of the above places is better than another for placement of it. So the selection of a location for placement of the it is totally dependent upon the preference of the neurosurgeon [5].
Time of shunt placement
Almost 80 percent of the patients with this condition need treatment and in most of the cases they are placed during the first days or weeks after birth. In some cases it is placed at the time of posterior fontanels closure [5].
Performing this operation on a baby with hydrocephalus
Clinical features of shunt malfunction
These include:
- Rapid increase in head size
- Fullness of fontanelle
- Irritability
- Recurrent vomiting
- Crossed eyes
- Sunset sign
- Periods of apnea
- Difficulty swallowing;
- A weak cry
- Difficulty in keeping the infant awake
- Any worsening brain function [6].
A head ultrasound, computed tomography (CT) scan or magnetic resonance imaging (MRI) scan can be used to check proper functioning of a shunt after its placement. Follow up visits of all patients with this condition should be carried out by a neurosurgeon at least every one to two years. Most of patients with this disability may require the shunt for their whole life [6].
Complications of surgery
As we mentioned this procedure is a kind of instrument that removes or drains extra or blocked fluid (CSF) from the brain. Like other medical instruments, complications may occur. Some complications are as follows:
- Failure or non functioning
- Blockage
- Headache, vomiting and nausea
- Seizures (either the onset of new seizures or an increase in the frequency of existing seizures)
- A significant alteration in intellect, school performance or personality
- Back pain
- Worsening arm or leg function
- Increasing scoliosis
- Worsening speech or swallowing issues
- Changes in bowel or bladder function
- Recurrent CNS and abdominal cavity infections [7].
Video of Surgery
Conclusion
Hydrocephalus shunts are commonly used to treat this condition. They are placed surgically between brain ventricles and some other part of body to drain the excessive CSF from brain to another part of the body. Thus they can drain CSF from the brain and prevent the complications of raised intracranial pressure. There are various types and the selection of their placement site is still under debate. Routine complications are infection, obstruction, and over drainage.
[ois skin=”1″]References
- Chumas P, Tyagi A, Livingston J. Hydrocephalus—what’s new? Arch Dis Child Fetal Neonatal Ed 2001; 85(3): F149–F154
- Bergsneider M, Egnor MR, Johnston M, et al. What we don’t (but should) know about hydrocephalus.J Neurosurg 2006;104(3 Suppl):157-9.
- Notarianni C, Vannemreddy P, Caldito G, et al.Congenital hydrocephalus and ventriculoperitoneal: influence of etiology and programmable on revisions. J Neurosurg Pediater. 2009;4(6):547-52.
- Watts C, Keith HD. Testing the hydrocephalus valve. Child Brain 1983;10(4):217-28.
- Sotelo J, Izurieta M, Arriada N. Treatment of hydrocephalus in adults by placement of an open ventricular. J Neurosurg 2001;94(6):873-9.
- Tuli S, Drake J, Lawless J, et al. Risk factors for repeated cerebrospinal failures in pediatric patients with hydrocephalus. J Neurosurg 2000;92(1):31-8.
- Schneider SJ, Wisoff JS, Epstein FJ. Complications of ventriculoperitoneal procedures or hydrocephalus associated with vein of Galen malformations in childhood.Neurosurgery 1992;30(5):706-8.