Spina bifida is a congenital birth defect that occurs due to the defective closure of bony component of vertebra during the intrauterine life. This birth defect may cause several complications in the patient. There is no cure of this birth defect but there are different treatment options available to help the management of the birth defect and decrease the complications.
Treatment before birth
Screening tests are performed in those mothers who are at the risk of having a baby with spina bifida. If spina bifida is diagnosed during the intra uterine life, there is an option to correct and treat the baby in the uterus during pregnancy to decrease the complications which develop due to defective spinal closure. The surgery is performed by the fetal surgeon. The risk assessment of mother and fetus is checked before performing the surgery. In this surgery, the defect is repaired and spinal cord is placed at its proper position.
Treatment after birth
There are several treatment options available for SB after the birth of the baby. It includes surgery, medical therapy, physical and behavior therapy. Treatment depends upon many factors such as given below:
- Type of the spina bifida
- Severity of the birth defect
- Age of the patient
- Health of the patient
- Personal preference
Treatment of spina bifida occulta
Spina bifida occulta is the mildest type of spina bifida. Sometimes, no treatment is required as the patient does not develop any complaint or any complications. If a patient develops any complication, it is treated accordingly.
Treatment of meningocele
Meningecele is a type of SB which presents with a sac on the back of patient. In this type, spinal cord or spinal nerves are not entrapped in the sac. There are two options to treat his type of the defect. These are following below:
- Removal of sac [1]
- Treatment of the complications developed due to this defect
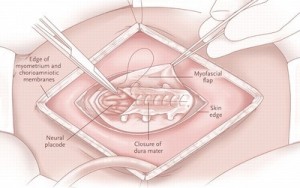
The sac is removed by a surgical procedure. Sometimes no complications develop due to meningocele. Removal of the sac is a kind of cosmetic surgery. If the size of sac is small, no surgery is performed. It is checked by an ultrasound to ensure that there is no spinal cord segment or spinal nerve, and then it is deflated by a syringe. The complications that are developed due to this defect include bladder problems, hydrocephalus or too much fluid in the brain.
Figure 1: Surgery for SB (Source: www.aboutspinabifida.blogspot.com)
Excessive fluid from the brain should be drained to decrease pressure on the brain tissue. In this surgery, a drain that is called shunt is placed under the skin from brain to the abdomen. By this shunt, excessive fluid is drained smoothly into the body fluid without causing any problem. Multiple surgeries are performed to adjust the function of drain. As the child grows, the position of the drain is changed. Again, surgery is performed to adjust the drain. It is done many times to prevent the development of hydrocephalus. If these complications are not treated, a patient may develop mental retardation or movement disorders. Some patients may develop paralysis of limbs and be unable to walk.
Treatment of myelomeningocele
Myelomenigocele is the worst type of spina bifida. In this type of SB, the spinal cord segment or spinal nerves protrude out through the defect of bony components of vertebra along with the protective coverings (meninges). It is a very complicated form of spina bifida and is associated with many complications.
The patients with myelomeningocele are prone to infection. So antibiotics are given to these patients to prevent infection.
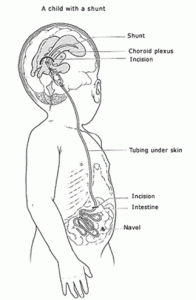
Hydrocephalus develops in these patients. It should be corrected to prevent mental retardation or movement disorders. A shunt is placed to drain the excessive fluid in the brain [2].
Figure 2: A child with shunt (Source: www.auniquelybeautifullife.weebly.com)
A very severe complication of this form of spina bifida is the progressive tethering of the spinal cord in which the spinal cord and vertebrae are not stretched and fail to grown properly as the child grows. Normally, the spinal cord is freely floating in the spinal cord. In tethered spinal cord, the spinal cord is attached to the spinal canal. Due to this attachment, compression is applied on the spinal nerves when spinal cord is stretched. This compression causes damage to the spinal nerves. When spinal nerves are damaged, the muscular function of bowel, bladder and legs are disturbed.
When the urinary bladder function is lost the patient is unable to void. Urinary retention develops and causes lower abdominal pain. An urologist is consulted for this problem. An urologist advises catheterization to drain the urine. In catheterization, a Foley’s catheter is passed in the urinary bladder through the urethra to drain urine. Repeated catheterization is a source of infection. Antibiotic cover is given along with catheterization.
Surgery is performed on the spinal cord to help restore the function of spinal nerves. Although surgery on spinal cord does not completely restore the function of spinal cord nerves, but it is helpful to improve the function and enhance the quality of life.
If SB involves the higher segments of the spinal cord, it is more dangerous and a patient is at a high risk of developing paralysis of lower limbs. Wheelchairs are used to help the patient in movement. If it involves the lower segments of the spinal cord then patient can walk independently or with the help of crutches.
Mobility and physical activity is helpful for the people who have developed movement disorders due to SB. Physical activity on a daily basis is recommended for every person but it is especially important for those people who are suffering from the movement disorders due to spina bifida.
Physiotherapy is very helpful for such patients. Physiotherapy enhances the activity of muscles. Physical activity is helpful to restore the function of paralyzed muscles. To enhance the physical activity, a patient is trained by a trained person. So that patient is able to do physical activity according to the need of the person.
References
- Tuzun Y, Izci Y, Polat KY. Anterior sacral meningocele: excision by the abdominal approach. Pediatr Neurosurg 2005;41(5):244-7.
- Warf B, Ondoma S, Kulkarni A, Donnelly R, Ampeire M, Akona J, et al. Neurocognitive outcome and ventricular volume in children with myelomeningocele treated for hydrocephalus in Uganda. J Neurosurg Padiatr 2009;4(6):564-70.