Spina bifida is a form of neural tube defect (NTD) that develops in the fetus during intra uterine life. Generally, every mother seems worried about her child whether the baby is normal or suffering from any congenital abnormality. Various screening spina bifida tests are performed during pregnancy to assess the baby while it is growing in its mother’s womb. If intrauterine screening tests are positive for spina bifida, many other confirmatory tests are also carried out because sometimes these confirmatory tests are positive but the baby is delivered as normal and has no defect. Even though these tests are negative, there is also a chance of having spina bifida in the baby but the chance is very low. Thus, to confirm the initial findings, false negative and false positive tests must be ruled out by performing some additional screening tests.
Blood tests for spina bifida
The following blood tests are performed for screening of spina bifida in the antenatal period, the period before the baby is born:
Maternal serum alpha fetoprotein test
This is a very common test used to check the NTDs in the developing baby. In this test, the mother’s blood is drawn and sent to the laboratory where alpha fetoprotein is checked in the serum of the blood sample [1]. Alpha fetoprotein is a protein that is produced by the baby in the cerebrospinal fluid. A small amount of it crosses through the placenta and appears in the mother’s blood. Normally it is not detected in the mother’s blood. When the baby is with NTDs, alpha fetoprotein found in the CSF achieves a free communication with the fluid which baths the child in uterus (amniotic fluid). From amniotic fluid, it crosses the placenta to reach the mother’s blood. High level of alpha fetoprotein detected in the serum of mother’s blood indicates a NTD is present in the fetus. As alpha fetoprotein is also raised in many other conditions such as liver cancer, testicular tumors and twin pregnancy. If a high level of AFP is detected, the test is repeated after some duration. If again the level is raised in the serum of mother’s blood, then confirmation is done by performing some other tests and ultrasonography.
Other blood tests
Other blood tests performed for screening of the spina bifida include the level of different hormones such as serum beta HCG level, inhibin A level and estriol level. These tests are called triple screen. These tests are not specific for NTDs.
Ultrasound
Ultrasonography is also used to screen the fetus for spina bifida [2]. If AFP level is found high in the mother’s blood, the obstetrician goes for ultrasonography to assure the presence of abnormality. With the help of the ultrasound scan, age of the developing baby and the total number of babies present in the uterus are identified. These two factors also disturb the AFP level. So, it must be determined why the AFP level is high. If gestational age is accurate and fetus is alone in the uterus, then high level of AFP is most probably due to spina bifida. High quality ultrasound scans by an expert sinologists get good images of the fetus in which spina bifida is identified. Severity of the spina bifida is also identified by the ultrasound scan of baby. It is the safest method to identify the problem for both mother and fetus. Ultrasound waves do not produce any harmful effects on the body of mother or the fetus. Most commonly ultrasound scans are performed two times during antenatal period. The first scan is done around the 8th to 14th week of gestation. During this scan, any problem with the spine of baby is indicated if the defect is of a severe type.
The second ultrasound scan is usually done around the 18th to 21st week of pregnancy. This scan is called anomaly scan. The main purpose of this scan is to identify any physical problem with the fetus. In this scan, spina bifida is easily identified.
Amniocentesis
Amniocentesis is the test that is performed on the amniotic fluid to detect the level of alpha fetoprotein in amniotic fluid. Amniotic fluid is obtained under the guidance of ultrasound. After aseptic measures, probe of the ultrasound is placed on the abdomen of the mother. The mother is placed in lateral position. In the position, maximum fluid collects on one side. The position of the fetus is assessed by the scan. A needle is inserted through the abdominal wall under the guidance of ultrasound. The needle reaches into the amniotic cavity. Amniotic fluid is aspirated and sent to the lab for the measurement of alpha fetoprotein level in amniotic fluid. Only a small amount of alpha fetoprotein is normally present in the amniotic fluid. A high level indicates the NTD in the fetus. The high level of alpha fetoprotein results because there is no skin present on the spine to cover it due to open spina bifida and hence alpha fetoprotein is leaked to the amniotic fluid. This test is mildly risky because there is mild risk for termination of pregnancy.
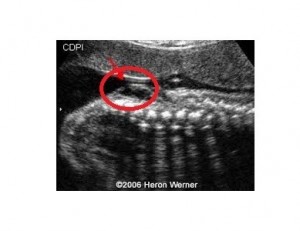
Figure 1: This picture was taken by ultrasound scan. In this picture, the fetus is shown in the uterus. A red circle is marked around the defect. Open neural tube defect is shown in the picture. Through this defect, free communication develops between the neural tube and amniotic sac (Source: www.sonoworld.com).
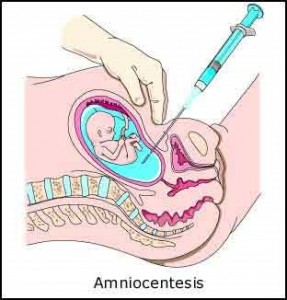
Figure 2: This is a picture of the amniocentesis test. In this picture, a needle is passed through the abdominal cavity to the amniotic cavity. With the needle amniotic fluid is being taken to measure the level of alpha fetoprotein (Source: www.irishhealth.com).
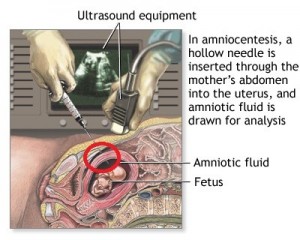
Figure 3: This is the picture of ultrasound guided amniocentesis. A needle is passed through the abdominal cavity to get amniotic fluid for analysis. The ultrasound probe is placed on the abdominal wall to assess the position of baby and amount of amniotic fluid (Source: www. pennstatehershey.adam.com).
References
- Bernard JP, Cuckle HS, Bernard MA, Brochet C, Salomon LJ, Ville Y. Combined screening for open spina bifida at 11-13 weeks using fetal biparietal diameter and maternal serum markers. Am J Obstet Gynecol 2013;209(3):223.e1-5.
- Bernard JP, Cuckle HS, Stirnemann JJ, Salomon LJ, Ville Y. Screening for fetal spina bifida by ultrasound examination in the first trimester of pregnancy using fetal biparietal diameter. Am J Obstet Gynecol 2012;207(4):306.e1-5.