Is spina bifida occulta bad?
Spina bifida (SB) is a type of neural tube defect (NTD) in which spine fails to enclose some of its bony components. SB is of many types. Spina bifida occulta (SBO) is one of the types and is considered the mildest form of spina bifida. Most of the time, it is missed or not diagnosed because it is covered by skin and no external deformity is seen. The meaning of occulta is hidden. It is hidden by the skin so it is called spina bifida occulta. The only finding in this condition is a small dimple on the skin, tuft of hairs or a red mark on the skin at the site of spinal defect. It can affect any vertebra in the spine but it usually affects the lower vertebra (lumber) of the spine.
It is often found accidently in a person when an x-ray, CT scan or MRI to diagnose another problem is performed for that person. Nothing but a small portion of missing vertebra is shown in the x-ray.
SBO is the most common and mildest type of Spina bifida, but the prevalence of this birth defect is still not known properly. According to surveys, about 22 percent to 23 percent people are living with SBO in the United Kingdom.
Complications and Symptoms
SBO is a form of spina bifida that is such a mild and simple type that it seldom shows symptoms that are associated with complications. Although there is a mild chance that a patient with SBO presents with a slipped disc and complains of pain radiating to the lower limbs. A slipped disc applies pressure on the associated spinal nerves [1]. Due to compression of spinal nerves, pain radiates to that region from where these nerves send signals. If a person during his or her childhood life has no complaint of SBO, he/she will never have any complaint in his adulthood life.
In SRO plates of bones that are helpful for the formation of the spinal arch cannot fuse completely. This form of spinal defect usually involves the one vertebra which often is the lowest vertebra of the spinal column. Because this form does not have any effect on the spinal cord or spinal nerves, there is no abnormality or problem associated with bladder, bowel and legs.
However, some patients present with other problems because these problems are related to condition where vertebra is not formed properly. For these people, this problem is more extensive with the spine as compared to the SBO.
If more than one vertebra is involved in the spina bifida lesion, it is referred as occulta spina dysraphism (OSD). This problem may cause the back of person to be little short and rigid. The usual curvature of the back may be overstated and there is abnormal and unusual curvature of the spine. There may be visible bony protrusion in the central line of the back of patient. A bony peg may be formed at some place in the spinal canal and a fibrous band may be formed across it dividing it in two parts. The spinal cord may become extremely wide due to the presence of unusual fibrous tissue in the spinal canal. Due to the disturbance of the spinal canal, the function of bladder, bowel and lower limbs may be affected.
Some other things that are related to this site and influence the normal function of person are given below:
- Disturbance of the spinal cord and spinal nerves coming out of the spine due to the tough (fibrous) tissues
- Tumors related to fat cells in the spine, beneath the skin or surrounding tissues
- Cysts around the spine under the skin
- Cysts filled with cerebrospinal fluid (CSF) in the affected site of spine
- Tethered spinal cord or attached to the walls of spinal canal
These structures are not visible and present internally. In addition to these structures, some signs are present on the skin and visible showing that there is underlying problem with the spinal cord. These signs are given below:
- A tuft of hair on the lower back of person
- A sinus tract visible on the skin from the skin surface down to the spinal cord
- A mass under the skin that is visible externally
- A undeveloped tail
- A bluish colored swelling over the lower part of spine called “capillary haemangioma”. It is most commonly present over the back of head and not associated with any risk.
Effects of Occulta Spina Dysraphism
As spinal nerves and roots are affected at the spot of lesion, it is said that any problem or disorder from the waist and below in the spine is most commonly due to OSD. The symptoms are mild, moderate and severe depending upon the amount of neural tissue association. The most common symptoms are mentioned below [2]:
- Muscular weakness of legs or feet
- Sensory loss in lower limbs
- Foot deformity
- Gait problems
- Problems associated with urinary tract system, i.e. incontinence
- Problems associated with bowl
- Abnormal curvature of the spine
- Back pain
Incontinence problem
If a child has incontinence, he/she can present with the problems given below:
- Bedwetting that is still present in the child after toilet training
- Not having awareness of when to pass the urine
- Inability to control the urine even for a few seconds
- Continuous dribbling of urine even after passing the urine
- Recurrent urinary tract infections (UTIs)
Lower Limb Problems
Most patients suffering from OSD have no problems with their lower limbs (muscles or bones). If any problem appears he/she is referred to an orthopedic surgeon for proper management.
Back Pain
Back pain is the most common complaint of every person in our society. Back pain due to OSD is difficult to identify and should be investigated to know the actual cause.
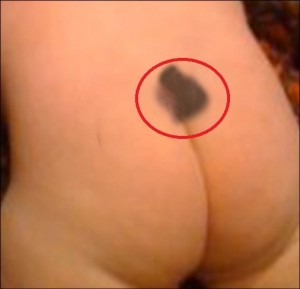
This is a picture of spina bifida occulta. A red circle is made around the tuft of hair present on the lower back of patient (Source: www.hello-berlin.net)
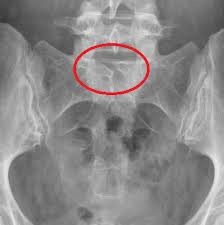
This is an x-ray film of spina bifida occulta. A red circle is made around the bony defect present in lumbar region (Source: www. doubtnichts.wordpress.com).
References
1. Srinivas S, Shetty R, Collins I. Symptomatic lumbar disc protrusion causing progressive myelopathy in a low-lying cord. Global Spine J 2012; 2(2):115–8,
Tavafoghi V, Ghandchi A, Hambrick GW Jr, Udverhelyi GB. Cutaneous signs of spinal dysraphism. Report of a patient with a tail-like lipoma and review of 200 cases in the literature. Arch Dermatol 1978;114(4):573-7.