Neural tube defect (NTDs) are the birth defects that occur due to faulty development of brain and spinal cord. These defects occur when the brain and spinal cord are not completely covered with membranes and bones, leaving the brain and spinal cord open [1]. NTDs occur in the 3rd week of pregnancy when some special type of cells on the dorsal aspect of the fetus begin to form the neural tube. The NTDs can be classified into two types, namely open NTDs and closed NTDs. Open NTDs are the most common type of these defects.
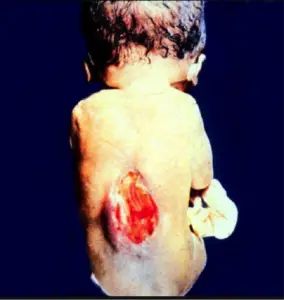
Source: www. hastane.deu.edu.tr
Incidence
NTDs are one of the most common congenital birth abnormalities, occurring in almost one in 1,000 live births in the United States. An NTD occurs very early in the developmental period since the neural tube is formed 28 days after conception. When the neural tube does not close adequately, a NTD develops. NTDs develop in the fetus before most women know they are even pregnant [2].
Types/examples of the Open Neural Tube Defect
As mentioned earlier, there are two types of NTDs, that is, open, which are more common and closed. A defect is said to be an open NTD if brain or spinal cord is exposed at birth through an opening in skull or vertebral column. Examples of open NTDs are given below [3]:
Anencephaly
The term anencephaly means “without head”. It is a type of open NTD’s that develop when the cranial end of the neural tube fails to close completely, usually during the 23rd and 26th days of pregnancy resulting in the lack of a major part of the brain and cranium. Infants born with this defect do not have the main parts of the forebrain and are usually blind, deaf and unconscious. Absence of forebrain part ensures that the baby will never gain consciousness [3,4]. Infants having this defect are either stillborn or usually die within a few hours or days after birth.
Encephaloceles
Encephalocele is another open neural type of defect which is characterized by herniation of a part of brain through the skull that is sac-like and covered with meninges. Encephaloceles can be classified into various types depending upon their location. Encephaloceles are often evident and diagnosed immediately. In some cases small encephaloceles remain undiagnosed [3,4].
Hydranecephaly
Hydranecephaly is an open type of NTD characterized by the absence of cerebral hemispheres; instead the skull is filled with sacs of cerebrospinal fluid [3].
Iniencephaly
Iniencephaly is a rare type of open NTD that causes an extreme bending of the head to the spine. Diagnosis of this abnormality can usually be made on antenatal ultrasonography; however, immediately after birth “the bent head with face looking superior” will indicate the diagnosis. Usually the neck is absent. The skin of the face connects directly to the chest and the scalp connects to the upper back. The infant will usually not survive more than a few hours [3,4].
Spina bifida is an NTD characterized by the incomplete closure of bone around the spinal cord resulting in a defect in the spinal cord. It can be further divided into two classes; spina bifida cystica and spina bifida occulta [3].
Spina Bifida Cystica
Spina bifida cystica can be further divided into two types, namely meningocele and myelomeningocele. Meningocele means herniation of the meninges (but not the spinal cord) through the defect in the spinal canal. Myelomeningocele means the protrusion of the meninges as well as the spinal cord through the opening [3,4].
Spina Bifida Occulta
By definition, spina bifida occulta refers to hidden split spine. In this NTD the spinous process and the neural arch appear abnormal on an X-rays, and are generally harmless. In most of the cases the spinal cord and spinal nerves are not involved [3,4].
Causes and risk factors of the Open Neural Tube Defects
The exact cause of NTDs is still under debate but there are certain environmental and genetic factors which are thought to be important in causation of NTDs. These are (5):
- Folic acid deficiency in the pregnant lady
- Use of certain drugs like anti-epileptics, methotrexate, etc
- Intake of mytoxins in contaminated corn meal
- Exposure or intake of arsenic
- Exposure to hyperthermia and radiation
- Previous history of NTDs
- Cigarette smoking
- Obesity
- Diabetes (5)
Diagnosis
NTDs in the antenatal period can be diagnosed with the following tests [6]:
- Ultrasonography
- Quadruple screening
- Serum alpha fetoprotein levels
- Amniocentesis
Diagnosis after birth can be made by:
- History and examination
- CT-head
- MRI-brain
- X-rays spine (6).
Treatment
There is no treatment available for anencephaly as the babies usually do not survive more than a few hours. There is certain role for aggressive surgical management in cases of spina bifida, meningoceles and mild myelomeningoceles. The outcome of surgical repair often depends on the amount of brain tissue involved in the encephalocele. The aim of treatment for NTDs is to allow the patient to achieve the maximum level of function [5,7].
Conclusion
Open neural tube defects are of various types. Folic acid deficiency in pregnant women and some genetic factors are involved in the causation of NTDs. Prognosis of NTDs depend upon the type of defect and adequate surgical treatment
[ois skin=”1″]
REFRENCES
- Copp AJ, Stanier P, Greene ND. Neural tube defects: recent advances, unsolved questions, and controversies. Lancet Neurol 2013;12(8):799-810.
- Persad VL, Hof M, Dube JM, Zimmer P. Incidence of open neural tube defects in Nova Scotia after folic acid fortification. CMAJ 2002; 167(3): 241–5.
- Imbruglia L, Cacciatore A, Carrara S. Abnormal skull findings in neural tube defects. J Prenat Med 2009 Jul-Sep; 3(3): 44–7.
- Saboval L, Horn F, Drdulova T, et al. [Clinical condition of patients with neural tube defects]. Rozhl Chir 2010;89(8):471-7.
- Manning SM, Jennings R, Madsen JR.Pathophysiology, prevention, and potential treatment of neural tube defects. Ment Retard Dev Disabil Res Rev 2000;6(1):6-14.
- Main MD, Mennuti MT. Neural tube defects: issues in prenatal diagnosis and counselling.Obstet Gynecol 1986;67(1):1-16.
- Phadke S, Agarwal M. Neural tube defects: A need for population-based prevention program. Indian J Hum Genet 2012; 18(2): 145-7.



