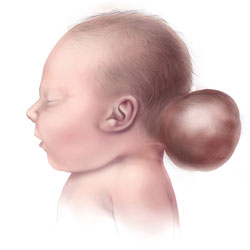
What is Encephalocele?
During fetal development when the neural tube fails to close completely it gives rise to an anomaly termed encephalocele. It is one of the important and well known causes of mortality and morbidity in infants1. It protrudes through the openings in the skull in the shape of cauliflower like protrusions of the brain and the membranes that cover it- that is, why it is also called cranium bifidum.
It can form a groove between forehead and nose, or on back of skull or in the middle of skull2. Recent studies show that it has more similarities with spina bifida (SB) than it has differences with it3.
Epidemiology
These anomalies are rare and occur at a rate of one in 5000 live births worldwide. In Europe and North America, the encephaloceles at the back of skull are more common while frontal encephaloceles are more frequently seen in Southeast Asia, Africa, Malaysia, and Russia. The occurrence of these anomalies are related to many factors like a family history of SB, parental age and some the ethnic, genetic and environmental factors4.
Classification
If the protruded part consists of only cerebrospinal fluid (CSF) with covering membranes, it may be termed as meningocele and but if the brain matter is also present, it may be called encephalomeningocele. It can be classified into the following5:
- Nasofrontal- between nose and front of head
- Nasoethmoidal- between nose and ethmoidal sinuses
- Naso-orbital- between nose and orbit
Causes
Recent studies show an association of these congenital anomalies with the following factors6:
- Exposure to cancer causing agents
- Exposure to tryptan blue- a stain used to color dead tissues
- Decreased level of folic acids
Clinical features
Babies with this anomaly can present with the following features6:
- Hydrocephalus– it refers to abundant CSF in the brain
- Weakness of limbs
- Micrecephaly- an abnormally small sized head
- Uncoordinated muscle movement
- Developmental delay
- Vision problems
- Mental and growth retardation
- Seizures
Various conditions may be associated with this congenital anomaly such as7:
- Meckel syndrome- it is characterized by the presence of occipital encephalocele along with micrecephaly, cleft palate, polycystic kidney disease, polydactyly and ambiguous genitals.
- Dandy-Walker-Malformation- it produces the enlargement of the 4th ventricle along with a cyst that extends into posterior cranial fossa.
- Chiari-Malformation- it is characterized by extension of the cerebellum into the spinal canal which blocks the flow of CSF.
- Chromosomal abnormalities (in almost40% of the cases)
Complications
This disability may cause7:
- Meningitis- it is usually a post operative complication which can be prevented by the use of antibiotics before and after surgery.
- Hydrocephalus– it can be treated by shunting or drainage of CSF.
- Blindness- it can occur as the vision center is present in the back of brain.
Dr. Meara, Boston Children’s Hospital talks about some complications
Management
In antenatal period, these anomalies can be diagnosed by ultrasonography. The typical ultrasonographic appearance of this anomaly is the presence of mass in the midline of the skull. Occasionally, a MRI may be needed for an accurate diagnosis. Alpha fetoprotein levels are usually not elevated. After birth, these anomalies can easily be diagnosed just by looking at them. A small encephalocele in the nasal or forehead region may not be detected. In such cases, physical and developmental delays can indicate the presence of this anomaly. Reparative surgery in infancy is the usual treatment of it6,7. During surgery following procedures are carried out:
- Reposition of the involved area
- Removal of protrusions
- Correction of deformities
- Relieving the CSF pressure
The recovery after surgery
The recovery of the patient after surgery depends upon different factors like age of the baby, size of it, involvement of brain tissue, location of it, extent of the repair and time spent in surgery. Most all babies need some breathing assistance after surgery that can be provided with the use of supplemental oxygen or by use of an endotracheal tube. Some babies may require total per-enteral nutrition after surgery for some time7.
Encephalocele prognosis
This congenital anomaly affects almost 375 babies per year in United States. About 20% of babies with it are delivered as still-born. About 21% of babies with this anomaly survive during the process of birth. Of those babies who born alive, only 50% survive. Location of the encephalocele is the major determinant of the prognosis of this disorder. Frontal encephalocele has the best prognosis (i.e., 100%). If they are present on the back of skull the survival rate is about 55%7.
A mother talks about her experience with this condition on the Jeremy Kyle talk show.
[ois skin=”1″]REFERENCES:
- Amadi CE, Eghwrudjakpor PO. The pattern of distribution of encephalocele in University of Port Harcourt Teaching Hospital–a three year experience. Niger J Med 2013;22(1):19-23.
- NINDS Encephaloceles Information Page [Internet]. 2007 [last updated 2007 Feb 17; cited 2013 Aug 17]. Available from: http://www.ninds.nih.gov/disorders/encephaloceles/encephaloceles.htm.
- Rowland CA, Correa A, Cragan JD, Alverson CJ. Are encephaloceles neural tube defects? Pediatrics 2006;118(3):916-23.
- Au KS, Ashley-Koch A, Northrup H. Epidemiologic and genetic aspects of spina bifida and other neural tube defects. Dev Disabil Res Rev. 2010;16(1):6-15.
- Khan AN, Encephalocele imaging: oTurnbull I, MacDonald S. verview [Internet]. 2011 [lasted updated 2011 May 25; cited 2013 Aug 17]. Available from: http://emedicine.medscape.com/article/403308-overview.
- Anthony D, John G, Adam R, Jeffrey V, Geoffrey L. Frontoethmoidal encephaloceles: reconstruction and refinements. J Caraniofac Surg 2011;12(1):6-18.
- What are Encephaloceles? [Internet]. [Cited 2013 Aug 17]. Available from: http://www.bandbacktogether.com/encephalocele-resources/.