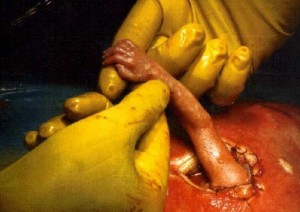
Overview
Prenatal surgical techniques for fetuses using animal models were first developed at the University of California, Sans Francisco in 1980 by Dr. Michael Harrison and his colleagues. The first human open fetal surgery in the world was also performed at the University of California, San Francisco under the direction and supervision of Dr. Michael Harrison on 26 April 1961 [1].
Fetal surgery includes a wide range of surgical procedures that are performed to treat birth defects such as spina bifida in fetuses, which are still in the pregnant uterus. Open fetal surgery and minimally invasive fetoscope surgery are well known procedures adopted for prenatal management of the fetuses suffering from neural tube defects (NTD’s). Open fetal surgery refers to complete opening of the uterus to operate on the fetus.
Minimally invasive fetoscope surgery is performed on fetuses by using small incisions, a fetoscope and sonography. In some cases, fetal surgery can be performed without incision or fetoscope; however, it is always performed with a real time cross-sectional view given by sonogram. As the fetal surgery for spina bifida is performed in antenatal period it is also called as prenatal spina bifida surgery operation [1,2].
Types of prenatal spina bifida surgery operations:
Open fetal surgery
Certain drugs called as tocolytics are generally administrated to the pregnant woman to prevent labor. However, these drugs should not be avoided in the presence of intrauterine infection, unexplained vaginal bleeding and fetal distress. The drug which reduces stomach acid secretion (like H2-antagonists) is usually given in the evening before and the morning of the operation plus an antacid like magnesium bicarbonate is usually administrated before induction to avoid the risk of acid aspiration. For sedation and intubation, a rapid sequence induction is used [5]. The following steps are performed during open fetal surgery:
- Opening the uterus by incision, called as hystertomy
- Exposing the fetus
- Performing surgical procedures on fetus to correct or repair spina bifida
- Returning the fetus back into the uterus
- Closing the uterus and abdominal wall
- Before applying the last stitch in the uterine wall, the amniotic fluid is replaced
The mother stays in the hospital for 3–7 days for pre-operative monitoring. Subsequently, a cesarean section is performed to deliver the baby. Remember babies who have been operated on for spina bifida or other birth defects are born preterm [5]. To perform fetal surgery, a surgeon has to achieve or maintain the following goals:
- Maternal safety should not be compromised at any cost during this surgery.
- Preterm labor should be avoided.
- The aims of the fetal surgery must be achieved [5].
Open fetal surgery if needed can be performed at any time between 18-30 weeks of gestation. However, open fetal surgery is not without risks. For example, the risk of premature labor is increased in the presence of certain risk factors such as multiple gestations, a history of maternal smoking, and very young or old mother. Open fetal surgery is quite safe for the mother, but for the fetus, safety is varies baby to baby and depends on the following factors:
- Types of specific procedure- different procedures have different advantages and disadvantages.
- The reasons for the procedure
- The gestational age of fetus
- Condition of the fetus [6].
The estimated overall perinatal mortality after open surgery is approximately 6%, according to a study in the United States 2003. It is also important to explain that all future pregnancies for the mother will require cesarean delivery because of the hysterotomy (performed during fetal surgery). Research reports show that there is no effect of fetal surgery on fertility of mother [3].
Indications of open fetal surgery include:
Prenatal repair of Neural Tube Defects like myelomeningocele and spina bifida is an important indication. The children treated with open fetal surgery have significantly improved prognosis compared to children whose defects are corrected shortly after birth. Prenatal fetal repair also decreases the need for ventriculoperitoneal shunt placement/dependence.
Children who have been operated on prenatally are twice as likely to walk independently at 30 months of age as children undergoing repair after delivery. Therefore, open fetal repair of spina bifida is the suggested standard of care at fetal specialty centers. Other indications for open fetal surgery include:
- Congenital heart diseases
- Pulmonary sequestration
- Saccrococcygeal teratoma
- Congenital diaphragmatic hernia [4].
Interview of couple who decided to undergo prenatal spina bifida surgery
Minimally invasive fetal surgery
A minimally-invasive fetoscope is a very small surgical instrument which is introduced into the uterus using real-time video imagery from fetoscopy and ultrasonography. This is a less invasive procedure than open fetal surgery. Some fetal surgeries can be performed with just a small guided wire sent percutaneously, while in other cases a small opening may be needed in the mother’s abdomen. Indications for minimally-invasive fetoscopic surgery include:
- Spina bifida
- Twin transfusion syndrome
- Fetal bladder obstructions
- Aortic or Pulmonary Valvuloplasty
- Atrial Septostomy
- Congenital diaphragmatic hernia [7].
Conclusion
There are various surgical techniques for antenatal repair of spina bifida. Many research reports show that the outcomes of prenatal fetal surgery are far better than those performed in the postnatal period. In other words, women at risk must be screened for neural tube defects and early management perhaps involving fetal surgery may be needed.
Excellent video on considering fetal surgery from the perspective of doctors
References
- Adzick NS. Fetal surgery for spina bifida: past, present, future. 2013;22(1):10-7.
- Sutton LN. Fetal surgery for neural tube defects. Best Pract Res Clin Obstet Gynaecol 2008;22(1):175-188.
- Deprest JA, Devlieger R, Srisupundit K, et al. Fetal surgery is a clinical reality. Semen Fetal Neonatal Med 2010;15(1):58-67.
- Kitano Y, Flake AW, Crombleholme TM, et al. Open fetal surgery for life-threatening fetal malformations. Semin Perinatol. 1999;23(6):448-61.
- Saxena KN. Anaesthesia for Fetal Surgeries. India J Anaesth. 2009;53(5):554-559.
- Zamora IJ, Ethun CG, Evans LM, et al. Maternal morbidity and reproductive outcomes related to fetal surgery. J Pediatr Surg 2013;48(5):951-5.
- Bui TH, Deprest JA, Ville Y, Westgren M. Minimally invasive techniques make fetal surgery possible. Disabling abnormalities can be corrected. Lakartidningen. 1998;95(44):4848-50,4853-4.
Related Articles:
- Cost of Treatments for Spina Bifida (incl Utero, Surgery, Therapy, etc)
- 15 Health Care Issues for Adults living with Spina Bifida
- 4 Facts about Spina Bifida Life Expectancy
- 5 issues with Spina Bifida Health Insurance
- How Spina Bifida Affects Childhood
- 6 Disorders Associated with Spina Bifida